-
-
Like what you see?
LetsTalkUrl
Let's Talk
From its beginnings in Wuhan, China and now dispersed to more than 120 countries, the novel Coronavirus (COVID-19) has infected over 660 million people with a death toll of over 6.6 million thus far. This makes it one of the deadliest outbreaks that the world has ever faced.
Compared to the double-stranded RNA viruses like HIV, Ebola, and Influenza, COVID-19, a single-strand RNA virus, mutates rapidly. This makes its spread more challenging to arrest. The virus is proving to be extremely difficult to analyze as well. Even if scientists develop a vaccine (which might take as much as 18 months or so), there is a chance that it may not be completely effective.
This is where AI can help. With the power and potential of next generation data science techniques and emerging technologies, healthcare agencies can effectively analyze, track and arrest the spread of coronaviruses like the COVID-19.
AI/machine learning algorithms can help fast-track genome sequence analysis, the drug development process, and development of an effective therapeutic regimen.
On the preventive side (which is the need of the hour), platforms that use advanced data science technologies can help agencies detect cases faster, predict new cases more accurately, monitor status, plan quarantines more effectively and arrest the spread of COVID-19. Here are some of the key components of such platforms.
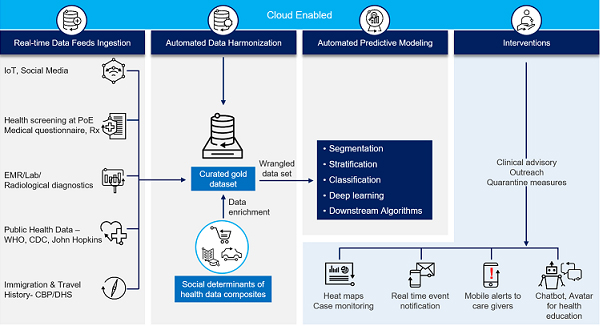
Data sources like IoT devices, systems that capture travel history and health symptoms at airports/ports of entry, social media updates, immigration information, public health data systems, transportation data, health insurance database, medical questionnaires, lab and radiological diagnostics and EHR can provide reams of data about people. This data can be key to generate the right intelligence to reduce the spread of COVID 19 or other epidemics. But how to manage this multi-format and multi-type data?
Agencies can automatically aggregate and store all this data using non-model databases. These databases fast-track data capture, ensure high operational speed, and provide greater analytical flexibility. Through process automation techniques, agencies can clean and harmonize all of this data in real-time, developing an integrated, unambiguous “golden record” of a person and the population quickly.
This data set can be further enriched with social determinants of health (SDOH) attributes. A person’s relationships, economic-behavioral- attitudinal composites (e.g. income, housing, state of hygiene, nature of work, access to care, propensity to engage with community, health awareness and engagement media preferences, etc.) shape health and disease distribution in the population. In the situations like COVID-19, SDOH data can help unearth additional information about a person/population, generating better intelligence to minimize the spread and raise awareness, particularly among the most vulnerable populations.
This SDOH enriched and harmonized data set can then be fed into an automated predictive modeling engine that can analyze various scenarios to proactively identify, assess and/or predict the at-risk people/population. The tool can generate proactive alerts and tailored recommendations to the care community. This analytical output can be also fed into a Chatbot/Avatar/Virtual Care Assistant solution or similar online communication tools to disseminate health education, preventive measure, quarantine, clinical advisory Q&As to the population and the care community.
Dynamic visualizations tools can make it easier for agencies to understand all this data. Agencies can visualize geo-clustering and heat mapping to track cases, events and locations related to the coronavirus. All this information can be further analyzed by advanced AI models to generate next-best-actions; i.e., automated recommendations for healthcare professionals in the care continuum to proactively determine the right interventions for the right people, just in time.
Related Read: Practicing Responsible Artificial Intelligence (AI)
FHIR (Fast Healthcare Interoperability Resources) compatibility and an API (Application Programming Interface) first approach will make the data and intelligence easily shareable across agencies and healthcare organizations for easy, near real time interventions and enable coordinated preventive measures for the population in need.
Cloud technology can host all these different components, making the platform easily accessible to the people in the field and scalable to meet changing requirements while staying compliant with strict healthcare regulations, including HIPAA and HITECH.
AI-based solutions like these can amplify the ability for an agency to more effectively fight deadly outbreaks like the novel coronavirus (COVID-19) and to ensure that the infected people receive the right care at the right time. It’s time for agencies to accelerate the adoption of AI-based technologies like Infosys Epidemic Surveillance Suite to fight pandemics like COVID-19 so that societies can more effectively deal with and control these outbreaks.

Dr. Suman is head of government healthcare analytics for Infosys Public Services. He has extensive experience in the public healthcare sector and previously worked for the World Health Organization, UNICEF and the Indian Public Health Association.
At Infosys, Dr. Suman leads the areas of vaccine management, advanced data science and artificial intelligence-enabled population health, social determinants of health analytics, opioid management, care management, and value-based care. He is a frequent public speaker at various healthcare conferences, forums and at major universities, including the Massachusetts Institute of Technology.
Dr. Suman is based in Hartford, Connecticut. He holds a medical degree from the University of Calcutta and master’s degree in healthcare administration from the Tata Institute of Social Sciences in Mumbai, India.